| |
| |
|
| |
Nevus of Ota |
| |
|
| |
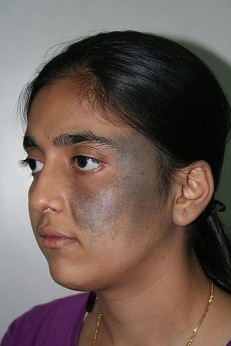
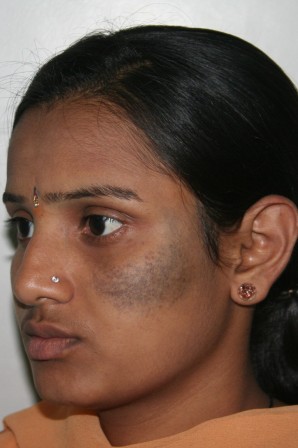
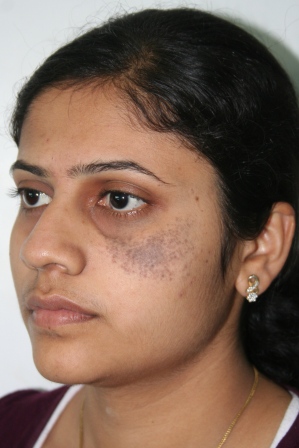
Nevus of Ota is a bluish or slate-gray hyper pigmentationthat occurs only on the face,usually on one side and rarely (5-10%) on both the sides.It is common in Asian patients and occurs as a result of entrapment of melanocytes (skin pigment producing cells) in the upper third of the dermis. |
| |
|
| |
Overview |
| |
It usually occurs on areas supplied by ophthalmic and maxillary divisions of the trigeminal nerve.This usually corresponds to forehead, scalp,temple, eyelids, cheeks, nose and ear. The sclera (white visible part of eye ball) is involved in two-thirds of cases.
In approximately 50-60% of the cases, the nevus is present at birth and in the remaining it develops during the first decade or during pubertyand adulthood.Nearly all lesions appear by the age of 30 years. Females are shown to be affected five times more than males.
Although this form of dermal melanocytosis may appear to be light in color during childhood, it can darken and spreadgradually as the person ages. Its color might also vary slightly depending on factors like weather conditions, hormones, or illness.However, the pigmentation doesn’t spread beyond the areas of the face supplied by the trigeminal nerve.
It is a benign condition, but may cause impairment in the quality of life due to the cosmetic disfigurement.
|
| |
|
| |
Background: |
| |
Nevus of Ota was first reported by Dr.M.T. Ota of Japan in 1939.
The exact cause of nevi of Ota and Ito are not known. Although unconfirmed, nevus of Ota and other dermal melanocytic disorders, such as nevus of Ito, blue nevus, and Mongolian spots, may represent melanocytes that have not migrated completely from the neural crest to the epidermis during the embryonic stage. The variable prevalence among different populations suggests genetic influences, although familial cases of nevus of Ota are exceedingly rare. The two peak ages of onset in early infancy and in early adolescence suggest that hormones are a factor in the development of these conditions.
Classification:
Nevus of Ota is classified into four types based on the extent of pigment localization and distribution:
o Type A has anperi-occular distribution. It is localized to the upper or lower eyelid or temporal region.
o Type B is localized to the zygomatic region.
o Type C is localized only to the forehead.
o Type D is localized only to the nasal ala.
- Type II (Moderate): Lesions may be distributed as those seen in type I, but to a more extensive degree.
- Type III (Intensive): Lesions have forehead, eyebrow, nose, and scalp involvement.
- Type IV (Bilateral): Lesions have a bilateral distribution.
|
| |
|
| |
Treatment:
|
| |
|
| |
The Q-switched 1064 nm Nd:YAGlaser is an ideal choice to treat dermal pigment as in nevus of Ota.Laser therapy tends to be most effective in individuals with lighter skin tones and in darker skin types it reduces the risk of epidermal injury and pigmentary alterations. Laser treatment destroys the excess melanocytes that cause the bluish hyperpigmentation, with a goal of returning the skin to its natural color.
The pigment clearance may be expected to be near total. Usually a number of treatment sessions with an interval of minimum six weeks are required to achieve total or near total clearance. The number of treatments depend mainly on the severity of the lesion. Darker the lesion, more are the treatments required. It also depends to some extent on the quality of the laser system used and its energy output. Last but not the least, experience of the laser surgeon plays a significant role in achieving early and good clearance.
|
| |
|
| |
Care & Aftercare
|
| |
|
| |
Immediately after laser treatment, patients will experience some stinging or burning sensation, which can be relieved by application of ice packs. There will be some amount of swelling which can last for a day or two. Bruising, if it occurs at places, usually settles in a few days on its own. Latter during the final few treatments, pin-point bleeding is expected as the amount of energy delivered needs to be increased to be effective. Usually this peels off as dry scabs without leaving any marks behind.
As is true with any cosmetic laser procedure, patients should protect the treated area of skin from sunlight throughout the period of treatment. This is best done by regular use of a sun block with a minimum SPF (Sun Protection Factor) of 45+. Additional use of physical protection in the form of a scarf, face-mask and umbrellas is helpful.
|
| |
|
| |
FAQs
|
| |
|
| |
Q : Is Nevus of Ota hereditary?
Nevus of Ota is a non-hereditary pigmentation disorder, which is more frequent in females than males. Unilateral presentation is typically seen, but bilateral involvement is described in 5–10% of patients.
Q :
Why its color changes its shades ?
After onset, nevus of Ota may slowly and progressively enlarge and darken in color, and its appearance usually remains stable once adulthood is reached. The color or perception of the color of nevus of Ota may fluctuate according to personal and environmental conditions, such as fatigue, menstruation, insomnia, and cloudy, cold, or hot weather conditions.
Q :
Should I visit ophthalmologist regularly ?
A reported 10% association of nevus of Ota with increased intraocular pressure warrants an ophthalmic consultation. The melanocytes that cause the hyperpigmentation can block the flow of fluids in the eye, raising the pressure inside the eye.It is important that patients become aware of the risk associated with the development of glaucoma as this may progress to vision loss. Periodic follow-up visits with an ophthalmologist are encouraged.
Q :
Is there any chance of developing cancer ?
Malignant degeneration of nevus of Ota is rare.Despite there being a rare risk of transformation into malignant melanoma, patients areadvised to report any changes in size and/or color to the lesional areas.
Q :
What is Nevus of Ito ?
Nevus of Ito, initially described by Minor Ito in 1954,is a similar dermal melanocytic condition like nevus of Ota, differing in distribution. Nevus of Ito is usually found distributed along the posterior supraclavicular and lateral cutaneous brachial nerves of the shoulder. Nevus of Ito often occurs in association with nevus of Ota in the same patient but is much less common, although the true incidence is unknown. From a pathophysiological standpoint, both nevus of Ota and Ito result from failed migration of melanocytes from the neural crest to basal layer of the epidermis.
Q :
What is Nevus of Hori ?
Nevus of Hori is a condition almost identical to nevus of Ota, which affects both sides of the face.
|
| |
|
| |
|
| |
|
| |
|
| |
|
| |
|
| |
|
|
|
 |